Endoscopic retrograde cholangiopancreatography (ERCP) is a minimally invasive endoscopic procedure that allows visualization and therapeutic maneuvers to be performed in the bile and pancreatic ducts. ERCP has traditionally been performed by reusable duodenoscopes, but disposable duodenoscopes have been introduced to the field in efforts to decrease endoscope-related infections. Traditional duodenoscopes require high-level disinfection due to their complex design, but residual bacteria can persist despite reprocessing. Sterile, disposable duodenoscopes reduce the risk of potential outbreaks and infections due to transmission, but these disposable duodenoscopes are costly and are associated with significantly more environmental waste and greenhouse gas emissions. This review will discuss the safety and efficacy of disposable duodenoscopes, their environmental impact, and potential indications for their use. Disposable gastroscopes will also be discussed.
INFECTION CONCERNS OF TRADITIONAL REUSABLE DUODENOSCOPES
Contamination Rates of Duodenoscopes
The incidence of infection following an ERCP ranges from 2-4%, and a small number of these infections can be attributed to exogenous causes related to contaminated reprocessed duodenoscopes transmitting organisms between patients. A study by Rauwers et al. found that 22% of reprocessed duodenoscope were contaminated and 15% of the duodenoscopes grew microorganisms with gastrointestinal or oral origin, including Enterobacter cloacae, Escherichia coli, Klebsiella pneumonia, and yeasts, many of which are part of the normal flora of the gastrointestinal tract. Another study found that reprocessed duodenoscopes could be contaminated at a rate of 5.3% with high-concern organisms, such as gram negative rods, Staphylococcus aureus, Staphylococcus lugdunensis, β-hemolytic Streptococcus, and Enterococcus species.
Endoscopic procedures are not sterile, and while efforts should be made to minimize endoscopy-related infections, equipment harboring bacteria does not guarantee that potentially harmful organisms will be transmitted to a patient. Currently, reusable duodenoscopes are used to perform most ERCPs in the United States and around the world, but their intricate structural design, especially the elevator mechanism, makes them difficult to successfully disinfect between procedures. For example, swabs of the elevator, distal end cap, and biopsy/suction channel had a higher probability of being contaminated.2 In addition to these factors related to the physical structure of a duodenoscope, Rauwers et al. identified miscommunication about reprocessing, undetected damaged parts, and inadequate repair of duodenoscope damage as potential reasons for outbreaks of multidrug resistant bacteria.

Post-Enhanced Surveillance and Reprocessing Techniques Rates
A meta-analysis conducted by Larson et al. found that there was a contamination rate of 15.25% for reprocessed, patient-ready duodenoscopes. Due to these contamination rates, in 2015 the United States Food and Drug Administration recommended enhanced surveillance and reprocessing techniques (ESRT) to improve disinfection. These additional reprocessing steps include microbiological culture, ethylene oxide sterilization, liquid chemical sterilant processing system, and double high-level disinfection. When ESRT protocols were followed, Bomman et al. found that the contamination rates were 5% and 0.8% for low and high-risk organisms, respectively.Although these enhanced techniques seem to lower contamination rates, reusable duodenoscopes are still unable to be completely sterilized, and disposable duodenoscopes have been developed as an alternative to mitigate this issue.
DISPOSABLE DUODENOSCOPES
Comparing Two Models
There are currently two disposable duodenoscopes commercially available in the United States, aScope Duodeno by Ambu Inc (Ballerup, Denmark) and EXALT Model D Single-Use Duodenoscope by Boston Scientific (Natick, Massachusetts), that are approved for clinical use by the FDA (Figures 1-7). Both are similar in design to currently available reusable duodenoscopes. A study completed by Shahid et al. compared the two disposable duodenoscopes and saw that they were rated similarly by endoscopists in terms of visualization quality, maneuverability, suction/air control, and elevator efficiency.This being said, however, endoscopists in this study rated both disposable duodenoscopes as inferior to their reusable counterparts.7

Safety and Efficacy
Both aScope Duodeno and EXALT Model D were found to have acceptable safety and efficacy.,, Bang et al. found that disposable duodenoscopes were comparable in terms of overall safety and technical performance to reusable duodenoscopes when performing low-complexity ERCP procedures.8 Specifically, Bang and colleagues found that there was no difference in maneuverability and the ability to provide therapeutic interventions, but ease of passage through the stomach, image quality, image stability, and air-water button functionality were inferior for disposable duodenoscopes when compared to reusable instruments. Although disposable duodenoscopes and reusable duodenoscopes may not perform identically, the overall safety and performance were felt sufficient to make disposable duodenoscopes a viable alternative to reusable ones when performing ERCP.
A comparative bench simulation study by Ross et al. found that completion times for disposable versus reusable duodenoscopes were comparable across 4 different tasks and 14 subtasks on anatomic bench models.9 There were no significant differences in performance between the disposable duodenoscope and the reusable duodenoscopes that were used.While this study found no significant difference in the overall performance rating of the different duodenoscopes, they noticed that the navigation/pushability ratings for the disposable duodenoscope was significantly lower than that of its reusable counterpart.
Fully disposable duodenoscopes were also successful in providing therapeutic interventions. A meta-analysis of 7 studies by Ramai et al. found high rates of success in cannulation (95%), sphincterotomy (100%), bile duct stone clearance (100%), stent placement (97%), stent removal (100%), and balloon dilation (97%).10 Overall, disposable duodenoscopes were comparable to reusable duodenoscopes and were able to achieve high rates of technical success.
Performance of Disposable Duodenoscopes in Complex ERCPs
Disposable duodenoscopes have also been successfully used in high complexity ECRPs with disposable duodenoscopes used to complete ERCP cases across all 4 American Society for Gastrointestinal Endoscopy (ASGE) complexity grades with overall completion rates of 96.7% and high median overall satisfaction rates.The performance of disposable duodenoscopes was seen to be effective and safe even during technically complicated procedures in a multicenter, international, retrospective study which evaluated 47 grade 3 and 19 grade 4 ERCPs and saw technical success rates of 98.5%.
Success with Non-Expert Endoscopists
Procedural outcomes are another potential concern surrounding disposable duodenoscopes when used by endoscopists with varying degrees of experience. A study by Slivka et al. compared outcomes for expert (as defined by >2000 lifetime ERCPs) and “less-expert” (lifetime ERCPS ≤ 2000) endoscopists and reported similar mean procedural completion times, mean number of cannulation attempts, crossover rate (crossover from a disposable device to a reusable duodenoscope), and proportion of cases with high complexity. This study found that both expert and less-expert endoscopists were able to use disposable duodenoscopes to successfully complete ERCPs with a range of complexity (all 4 ASGE complexity grades). ERCP completion rate and median completion time for expert vs. less-expert endoscopists were 96.3% vs. 97.5% and 25.0 vs. 28.5 minutes, respectively. The median overall satisfaction with the disposable duodenoscopes were similar for the two groups as well. A study by Bruno et al. similarly found good ERCP procedural success and high-performance ratings for disposable duodenoscopes used by endoscopists with varying levels of experience across academic medical centers in 11 countries.

ADVERSE EVENTS REPORTED WITH DISPOSABLE DUODENOSCOPES
Infections
Disposable duodenoscopes are delivered in a sterile package. Endoscope-related infections, however, are not only caused by transmission of bacteria from reusable duodenoscopes and can also occur due to endogenous bacteria transmitted from a patient’s mouth or upper GI tract to their biliary tract. A meta-analysis including only studies of ERCPs completed with disposable duodenoscopes still included the adverse event of post-ERCP infection.11 As such, it should be emphasized that even completely sterile instruments do not eliminate the possibility of ERCP-related infection.
Other Adverse Events
Disposable duodenoscopes may decrease the chances of endoscope-related infections, but the differences in tactile feedback, navigation, and so-called “pushability” of these newer devices may also make them susceptible to contributing to other ERCP associated adverse events. This is evidenced by a case report of an esophageal perforation during an ERCP using a disposable duodenoscope performed by an experienced endoscopist at a community hospital.18 An analysis of post marketing surveillance data of disposable duodenoscopes from 2018 to 2021 also found 3 reports of internal organ perforation, 2 reports of tissue damage, and 2 reports of hemorrhage or bleeding.
In addition to patient-related adverse events, there are also reports of device failures. There were reports of optical problems, difficulty advancing the duodenoscope, fluid leaks, and use-of-device problems.16 Endoscopists should be aware of these issues when using disposable duodenoscopes. Differences in feel and device operational properties can lead to adverse patient events, and more research needs to be conducted to see if these are being caused by unfamiliarity with the device or due to differences in device design, tactile feedback, materials, or other characteristics.
DISPOSABLE GASTROSCOPES
In addition to disposable duodenoscopes, disposable gastroscopes are available. Reusable gastroscopes can also be contaminated with native flora of a patient, and the incidence of infectious transmission by gastroscope is reported to be between 1.6 and 3.7 per 1,000 gastrointestinal endoscopic procedures. Duodenoscopes are prone to reprocessing errors because of their complex designs, but Goyal et al. found that there was a 19.98% contamination rate unrelated to the elevator mechanism in gastrointestinal endoscopes. The authors’ meta-analysis including only studies evaluating gastroscopes found a contamination rate of 28.22% ± 0.076%. Like disposable duodenoscopes, disposable gastroscopes may decrease procedure-related infections. These devices may also be advantageous in the ICU, OR, or other settings beyond GI endoscopy suites.

A study by Li et al. reported that disposable endoscopes had similar rates of excellent and good image qualities when compared to the traditional endoscopes.15 The maneuverability satisfaction of disposable endoscopes was also not inferior to the conventional reusable endoscope. There was no significant difference observed in endoscopy outcomes or adverse events, but the procedure duration for the disposable endoscope was longer (8.40 ± 4.28 vs. 5.12 ±2.65). Han et al. conducted at pilot study of 30 patients who underwent diagnosis and/or treatment with a disposable esophagogastroduodenoscopy (EGD). Therapeutic EGD was performed on 13 of the patients and included hemostasis, foreign body retrieval, nasoenteric tube placement, and percutaneous endoscopic gastrostomy. All procedures were successfully completed without crossover to a conventional, reusable gastroscope, and the authors concluded that the EGD using the disposable scope may be a feasible alternative in emergency, bedside, and intraoperative settings.
COSTS AND EFFORTS TO CLEAN REUSABLE DUODENOSCOPES
Costs to Clean
One benefit of disposable duodenoscopes is that they eliminate the need for and cost of duodenoscope reprocessing. Compared to standard reprocessing techniques, Bomman et al. found that enhanced reprocessing costs were 2.6-fold higher with “culture and quarantine” and 3.7-fold higher with the EtO sterilization technique. More specifically, at these institutions, the adoption of double high-level disinfection (HLD) increased the costs by about 47% ($80 vs. $118) in comparison to single HLD. Culture and quarantine increased costs by 160% ($80 vs. $208) and ethylene oxide (EtO) gas sterilization increased costs by 270% ($80 vs. $296). Based on their analysis, the authors found that the implementation of enhanced-SRT would require an additional annual budget of $406,000 for high volume centers. In addition to the increased costs, enhanced-SRT introduced significant scope downtime, which created a 3.4-fold increase in the number of scopes needed to keep up with the procedural volume at these centers.While enhanced surveillance and reprocessing techniques lower contamination rates, they come with additional costs and labor.
Barakat et al. found that partially disposable duodenoscopes (duodenoscopes with disposable endcaps) were the most favorable from a cost utility standpoint when downstream costs associated with duodenoscope-transmitted infection were taken into account. They also noted that disposable duodenoscopes were a more favorable option from a cost utility standpoint when compared to single or double HLD, EtO sterilization, and culture and quarantine. Even in low-volume settings (centers performing fewer than 50 ERCPs a year), they found that partially disposable duodenoscopes were the most favorable in terms of cost-utility, followed by culture and quarantine, EtO sterilization, double HLD, single HLD as the least favorable.
Efforts to Clean
In addition to the high costs required to maintain reusable duodenoscopes, reprocessing them also takes considerable time and manual effort. A survey by Sivek et al. reported that it takes ≤ 10 minutes to finish pre-cleaning and 16 to 30 minutes to finish manual cleaning. This study found that the top 3 contributing factors to cleaning difficulty were time pressure, small cleaning areas, and uncomfortable height of work surfaces for operators. Factors contributing to reduced cleaning effectiveness similarly involved time pressure, uncomfortable height work surfaces, quality of training, and memory load (remembering all the steps of the cleaning process). Cleaning reusable duodenoscopes, depending on the model, takes about 18-23 steps for the pre-cleaning process and about 60-85 steps for the manual cleaning procedure. These cleaning procedures were also reported to cause body fatigue or discomfort for ≥75% of respondents. If reusable duodenoscopes continue to be the main type of duodenoscope used, these human factor issues should be addressed to provide a better work environment that can hopefully lead to lower contamination rates.
ENVIRONMENTAL EFFECTS OF DISPOSABLE DUODENOSCOPES
4.4% of total greenhouse gas emissions worldwide and 8% in the United States are due to the healthcare sector. Eighteen million endoscopic procedures are performed in the United States each year, and endoscopy has a considerable impact on the environment. While disposable duodenoscopes decrease concerns for procedure-related infections, increased utilization will also increase the amount of waste generated from disposable instruments.
After completing a 5-day cross-sectional study at two US academic medical centers, Namburar et al. reported that a single endoscopy (assuming disposable endoscopes have the same mass as reusable endoscopes) generated 2.1 kg of disposable waste (2.4 kg when including waste from reprocessing).21 64% of the waste was destined for the landfill, 28% of waste was biohazard waste, and 9% was recycled. Over a five-day period, 278 endoscopies were performed at these two medical centers and the total waste produced amounted to a remarkable 619 kg.
When applying these estimates to all endoscopic procedures performed in the United States annually, the total waste produced from single-use supplies would weigh 38,100 metric tons, the equivalent of covering 117 soccer fields with waste coming up to 1 m.21 When adding the additional waste produced when reprocessing endoscopes, the total waste mass increases to 43,500 metric tons, and the total waste volume would cover 130 soccer fields.
If colonoscopies and ERCPs, to name just two endoscopic procedures, were performed solely by disposable endoscopes, the waste related to reprocessing would decrease, but the total net waste mass per endoscopic procedure would increase by 25%.21 Even after accounting for the lack of waste generated from reprocessing, using disposable endoscopes would increase the total net waste mass by 40%. The authors found that disposable endoscopes would create about 2 kg of waste per procedure, and only 10% of the waste was actually recycled. Disposable endoscopes would negatively impact the environment by creating more greenhouse gas emissions via the incineration of plastic material. The environment can also be expected to be impacted from the manufacturing of the disposable endoscopes.
For each reusable endoscope, approximately 2,000 disposable endoscopes need to be produced to perform an equal number of procedures.21 This is due to the fact that reusable endoscopes are designed to have a multi-year lifespan and are manufactured to stand up to repeated uses that involve significant mechanical forces. Le et al. estimated that performing an ERCP with a disposable duodenoscope releases between 36.6 and 71.5 kg CO2 equivalent.22 This is a staggering 24 to 47 times more than the emissions emitted with the use of a reusable duodenoscope or a reusable duodenoscope with a disposable endcap. Manufacturing disposable duodenoscopes accounts for 91% to 96% of these emissions. Although reprocessing reusable duodenoscopes generates greenhouse emissions, the top contributor of emissions for these scopes is electricity use during the procedure. In comparison to reusable duodenoscopes, Le et al. estimated that disposable duodenoscopes have 4 times higher ecosystem impact (expressed as the number of potentially lost species) than reusable duodenoscopes and consume at least 26 times more resources, even after reprocessing was taken into account.
Reusable duodenoscopes carry a higher rate of contamination after reprocessing, but Le et al. found that disposable duodenoscopes have 13 to 26 times more impact than reusable duodenoscopes in terms of environmentally mediated human health impacts, 4 to 7.5 times more impact in regards to ecosystem quality, and 26 to 50 times more impact when looking at resource consumption.21 Disposable duodenoscopes can provide a public health benefit by decreasing potential infections and infectious transmissions between patients, but this comes at a higher cost to the environment.
INDICATIONS FOR DISPOSABLE DUODENOSCOPES
Low Volume Institutions
Bang et al. looked at the per-procedure cost of a disposable duodenoscope in the United Sates and found that the costs can vary from $797 to $1547 for centers performing at the 75th percentile of ERCP procedure volume (125-150 ERCPs per year) and from $1318 to $2068 for institutions performing at the 25th percentile of ERCP procedural volume (≤50 ERCPs per year) based on infection rates. When infections were not factored, the per-procedure cost decreased to $818 and $297 for centers performing at the 25th and 75th percentiles, respectively, suggesting that the cost of a disposable duodenoscope differs depending on both infection rates and procedure volume.
Based on this analysis, for a large-volume center to break even, disposable duodenoscopes would need to be priced much lower compared to low-volume centers. While this ‘per procedure cost’ will differ depending on the center, at the authors’ institution, a reusable duodenoscope purchased for $35,000 was used for 3 years to perform about 200 ERCPs each year. If a disposable duodenoscope was used in its place, it would cost about $367,200 ($612 per procedure), which would be over 10 times the costs to perform the same number of ERCPs using a reusable duodenoscope. Low volume centers that have technical expertise but that do not want to invest in capital equipment may be more inclined to incorporate the use of disposable duodenoscopes.
High Risk Patients
Reusable duodenoscopes may harbor bacteria even after reprocessing, but it is unclear how frequently this translates to patient infections. A majority of post-ERCP infections are likely due to suboptimal ductal drainage and residual microbes, so the number of infections directly caused by contaminated duodenoscopes is uncertain.22
An analysis of Fee-for-Service Medicare patients undergoing ERCP identified 823,575 procedures between January 2015 and December 2021 and found that 3.5% (29,090) of these patients were hospitalized for infection within 7 days of the ERCP. Disposable duodenoscopes were billed for 711 of the procedures, and there was a 1.4% post-ERCP infection rate within 7 days. This study demonstrates that disposable duodenoscopes decrease the number of post-ERCP infections, but do not eliminate them completely. The analysis also found that ERCPs that were performed for urgent indications were the strongest risk factor for infections within the 7-day period. Chronic conditions, infection at time of ERCP, male sex, older age, and race were also risk factors. Disposable duodenoscopes did not fully eliminate post-ERCP infections in this study, but it may be appropriate to consider disposable duodenoscopes in patient populations that are at higher risk for post-ERCP infection, targeting these groups for specialized infection control prevention measures to avoid both duodenoscope-transmission of high-risk organisms to these patients and contamination of duodenoscopes.
CONCLUSION
Reusable duodenoscopes have been shown to harbor bacteria after reprocessing, and a small number of endoscope-related infections are thought to be due to transmission between patients via contaminated devices. Enhanced surveillance and reprocessing techniques can lower contamination rates significantly, but do not fully eliminate the risk. For this reason, disposable duodenoscopes have become available as a solution. Currently, two models are available and it is likely more will follow from other manufacturers.
Disposable duodenoscopes have acceptable safety and efficacy and can be considered as an alternative to reusable duodenoscopes for ERCP. However, the effects of disposable duodenoscopes on post-ERCP infection rates have not been clearly studied and larger studies are still needed.
Disposable duodenoscopes generate significantly more waste and greenhouse gas emissions than reusable duodenoscopes. Their effect on the environment will be determined by how widely they are adopted. Although studies have shown that low volume institutions may be more inclined to use disposable duodenoscopes and that certain patient populations may preferentially benefit from them, more time and research is needed to determine when disposable duodenoscopes should be used and if the incremental health benefit is worth the substantially higher cost to the environment.
References
References
Kovaleva J, Peters FT, van der Mei HC, Degener JE. Transmission of infection by flexible gastrointestinal endoscopy and bronchoscopy. Clin Microbiol Rev. 2013 Apr;26(2):231-54. doi: 10.1128/CMR.00085-12. PMID: 23554415; PMCID: PMC3623380.
Rauwers AW, Voor In ‘t Holt AF, Buijs JG, de Groot W, Hansen BE, Bruno MJ, Vos MC. High prevalence rate of digestive tract bacteria in duodenoscopes: a nationwide study. Gut. 2018 Sep;67(9):1637-1645. doi: 10.1136/gutjnl-2017-315082. Epub 2018 Apr 10. PMID: 29636382; PMCID: PMC6109280
Okamoto N, Sczaniecka A, Hirano M, Benedict M, Baba S, Horino Y, Takenouchi M, Morizane Y, Yana I, Segan R, Pineau L, Alfa MJ. A prospective, multicenter, clinical study of duodenoscope contamination after reprocessing. Infect Control Hosp Epidemiol. 2022 Dec;43(12):1901-1909. doi: 10.1017/ice.2021.525. Epub 2022 Mar 18. PMID: 35300743; PMCID: PMC9753065.
Rauwers AW, Troelstra A, Fluit AC, Wissink C, Loeve AJ, Vleggaar FP, Bruno MJ, Vos MC, Bode LG, Monkelbaan JF. Independent root-cause analysis of contributing factors, including dismantling of 2 duodenoscopes, to investigate an outbreak of multidrug-resistant Klebsiella pneumoniae. Gastrointest Endosc. 2019 Nov;90(5):793-804. doi: 10.1016/j.gie.2019.05.016. Epub 2019 May 15. PMID: 31102643.
Larsen S, Russell RV, Ockert LK, Spanos S, Travis HS, Ehlers LH, Mærkedahl A. Rate and impact of duodenoscope contamination: A systematic review and meta-analysis. EClinicalMedicine. 2020 Jul 15;25:100451. doi: 10.1016/j.eclinm.2020.100451. PMID: 32954234; PMCID: PMC7486302.
Bomman S, Ashat M, Nagra N, Jayaraj M, Chandra S, Kozarek RA, Ross A, Krishnamoorthi R. Contamination Rates in Duodenoscopes Reprocessed Using Enhanced Surveillance and Reprocessing Techniques: A Systematic Review and Meta-Analysis. Clin Endosc. 2022 Jan;55(1):33-40. doi: 10.5946/ce.2021.212. Epub 2022 Jan 3. PMID: 34974676; PMCID: PMC8831410.
Shahid HM, Bareket R, Tyberg A, Sarkar A, Simon A, Gurram K, Gress FG, Bhenswala P, Chalikonda D, Loren DE, Kowalski TE, Kumar A, Vareedayah AA, Abhyankar PR, Parker K, Gabr MM, Nieto J, De Latour R, Zolotarevsky M 5th, Barber J, Zolotarevsky E, Vazquez-Sequeiros E, Gaidhane M, Andalib I, Kahaleh M. Comparing the Safety and Efficacy of Two Commercially Available Single-Use Duodenoscopes: A Multicenter Study. J Clin Gastroenterol. 2023 Sep 1;57(8):798-803. doi: 10.1097/MCG.0000000000001752. PMID: 35997700.
Bang JY, Hawes R, Varadarajulu S. Equivalent performance of single-use and reusable duodenoscopes in a randomised trial. Gut. 2021 May;70(5):838-844. doi: 10.1136/gutjnl-2020-321836. Epub 2020 Sep 7. PMID: 32895332; PMCID: PMC8040157.
Ross AS, Bruno MJ, Kozarek RA, Petersen BT, Pleskow DK, Sejpal DV, Slivka A, Moore D, Panduro K, Peetermans JA, Insull J, Rousseau MJ, Tirrell GP, Muthusamy VR. Novel single-use duodenoscope compared with 3 models of reusable duodenoscopes for ERCP: a randomized bench-model comparison.
Ramai D, Smit E, Kani HT, Papaefthymiou A, Warner L, Chandan S, Dhindsa B, Facciorusso A, Gkolfakis P, Ofosu A, Barakat M, Adler DG. Cannulation rates and technical performance evaluation of commericially available single-use duodenoscopes for endoscopic retrograde cholangiopancreatography: A systematic review and meta-analysis. Dig Liver Dis. 2023 Mar 30:S1590-8658(23)00513-3. doi: 10.1016/j.dld.2023.02.022. Epub ahead of print. PMID: 37003844.
Muthusamy VR, Bruno MJ, Kozarek RA, Petersen BT, Pleskow DK, Sejpal DV, Slivka A, Peetermans JA, Rousseau MJ, Tirrell GP, Ross AS. Clinical Evaluation of a Single-Use Duodenoscope for Endoscopic Retrograde Cholangiopancreatography. Clin Gastroenterol Hepatol. 2020 Aug;18(9):2108-2117.e3. doi: 10.1016/j.cgh.2019.10.052. Epub 2019 Nov 6. PMID: 31706060.
Fugazza A, Colombo M, Kahaleh M, Muthusamy VR, Benjamin B, Laleman W, Barbera C, Fabbri C, Nieto J, Al-Lehibi A, Ramchandani M, Tyberg A, Shahid H, Sarkar A, Ehrlich D, Sherman S, Binda C, Spadaccini M, Iannone A, Khalaf K, Reddy N, Anderloni A, Repici A. The outcomes and safety of patients undergoing endoscopic retrograde cholangiopancreatography combining a single-use cholangioscope and a single-use duodenoscope: A multicenter retrospective international study. Hepatobiliary Pancreat Dis Int. 2023 Apr 11:S1499-3872(23)00047-4. doi: 10.1016/j.hbpd.2023.04.002. Epub ahead of print. PMID: 37100688
Slivka A, Ross AS, Sejpal DV, Petersen BT, Bruno MJ, Pleskow DK, Muthusamy VR, Chennat JS, Krishnamoorthi R, Lee C, Martin JA, Poley JW, Cohen JM, Thaker AM, Peetermans JA, Rousseau MJ, Tirrell GP, Kozarek RA; EXALT Single-use Duodenoscope Study Group. Single-use duodenoscope for ERCP performed by endoscopists with a range of experience in procedures of variable complexity. Gastrointest Endosc. 2021 Dec;94(6):1046-1055. doi: 10.1016/j.gie.2021.06.017. Epub 2021 Jun 26. PMID: 34186052.
Bruno MJ, Beyna T, Carr-Locke D, Chahal P, Costamagna G, Devereaux B, Giovannini M, Goenka MK, Khor C, Lau J, May G, Muthusamy VR, Patel S, Petersen BT, Pleskow DK, Raijman I, Reddy DN, Repici A, Ross AS, Sejpal DV, Sherman S, Siddiqui UD, Ziady C, Peetermans JA, Rousseau MJ, Slivka A; EXALT Single-use Duodenoscope Study Group. Global prospective case series of ERCPs using a single-use duodenoscope. Endoscopy. 2023 Sep 20. doi: 10.1055/a-2131-7180. Epub ahead of print. PMID: 37463599
Cheema BS, Ghali M, Schey R, Awad Z, Ribeiro B. Esophageal Perforation after Using a Single-Use Disposable Duodenoscope. Case Rep Gastroenterol. 2021 Dec 23;15(3):972-977. doi: 10.1159/000519685. PMID: 35110984; PMCID: PMC8787548.
Ofosu A, Ramai D, Mozell D, Facciorusso A, Juakiem W, Adler DG, Barakat MT. Analysis of reported adverse events related to single-use duodenoscopes and duodenoscopes with detachable endcaps. Gastrointest Endosc. 2022 Jul;96(1):67-72. doi: 10.1016/j.gie.2022.02.013. Epub 2022 Feb 17. PMID: 35183542.
Li DF, Shi RY, Tian YH, Xu ZL, Zhou YS, Sun XJ, Cai JW, Fang YY, Peng H, Wang JM, Dong T, Cai YD, Yao J, Wang LS. The feasibility and safety of disposable endoscope vs. conventional endoscope for upper gastrointestinal tract examination: a multicenter, randomized, parallel, non-inferiority trial. Z Gastroenterol. 2022 Sep;60(9):1314-1319. doi: 10.1055/a-1555-0568. Epub 2021 Nov 12. PMID: 34768288; PMCID: PMC9477113.
Goyal H, Larsen S, Perisetti A, Larsen NB, Ockert LK, Adamsen S, Tharian B, Thosani N. Gastrointestinal endoscope contamination rates – elevators are not only to blame: a systematic review and meta-analysis. Endosc Int Open. 2022 Jun 10;10(6):E840-E853. doi: 10.1055/a-1795-8883. PMID: 35692921; PMCID: PMC9187382.
Han ZL, Lin BT, Wang ZJ, Chen X, Xi YY, Wang JF, Qiao WG, Huang Y, Lin ZZ, Huang SH, Chua TY, Liu SD, Luo XB. Evaluation of a novel disposable esophagogastroduodenoscopy system in emergency, bedside, and intraoperative settings: Pilot study (with videos). Dig Endosc. 2023 Nov;35(7):857-865. doi: 10.1111/den.14548. Epub 2023 Apr 5. PMID: 36905288.
Bomman S, Kozarek RA, Thaker AM, Kodama C, Muthusamy VR, Ross AS, Krishnamoorthi R. Economic burden of enhanced practices of duodenoscopes reprocessing and surveillance: balancing risk and cost containment. Endosc Int Open. 2021 Aug 23;9(9):E1404-E1412. doi: 10.1055/a-1515-2591. PMID: 34466366; PMCID: PMC8382507.
Barakat MT, Ghosh S, Banerjee S. Cost utility analysis of strategies for minimizing risk of duodenoscope-related infections. Gastrointest Endosc. 2022 May;95(5):929-938.e2. doi: 10.1016/j.gie.2022.01.002. Epub 2022 Jan 10. PMID: 35026281.
Sivek AD, Davis J, Tremoulet P, Smith M, Lavanchy C, Sparnon E, Kommala D. Healthcare worker feedback on duodenoscope reprocessing workflow and ergonomics. Am J Infect Control. 2022 Sep;50(9):1038-1048. doi: 10.1016/j.ajic.2022.01.012. Epub 2022 Jan 30. PMID: 35108583
Namburar S, von Renteln D, Damianos J, Bradish L, Barrett J, Aguilera-Fish A, Cushman-Roisin B, Pohl H. Estimating the environmental impact of disposable endoscopic equipment and endoscopes. Gut. 2022 Jul;71(7):1326-1331. doi: 10.1136/gutjnl-2021-324729. Epub 2021 Dec 1. PMID: 34853058
Bang JY, Sutton B, Hawes R, Varadarajulu S. Concept of disposable duodenoscope: at what cost? Gut. 2019 Nov;68(11):1915-1917. doi: 10.1136/gutjnl-2019-318227. Epub 2019 Feb 12. PMID: 30772837; PMCID: PMC6839801.
Hutfless S, Shiratori Y, Chu D, Liu S, Kalloo A. Risk factors for infections after endoscopic retrograde cholangiopancreatography (ERCP): a retrospective cohort analysis of US Medicare Fee-For-Service claims, 2015-2021. BMJ Open. 2022 Sep 9;12(9):e065077. doi: 10.1136/bmjopen-2022-065077. PMID: 36691191; PMCID: PMC9472111.
 Monique T. Barakat
Monique T. Barakat Douglas G. Adler
Douglas G. Adler Yichun Fu
Yichun Fu Dejan Micic
Dejan Micic Miguel Regueiro
Miguel Regueiro Benjamin Cohen
Benjamin Cohen Ravi S. Shah
Ravi S. Shah


 Elliot B. Tapper
Elliot B. Tapper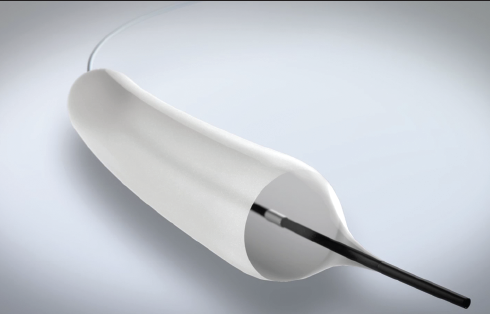
 Uma Mahadevan
Uma Mahadevan Courtney Walker
Courtney Walker



 Greta Macaire
Greta Macaire